Our goal in creating a value-based purchasing (VBP) model is to improve the quality of care and health for our members while lowering costs. VBP rewards providers for delivering high‑quality, efficient care instead of paying only for the number of services they provide.

What is Value-Based Purchasing?
Value-Based Purchasing
Focus: Quality
- Better patient health
- Fewer complications
- Improved outcomes
Result: Better results = Better pay
(Pays for quality)
compared to Traditional Payment⇢
Traditional Payment (Fee-for-Service)
Focus: Volume
- More appointments
- More tests
- More procedures
Result: More services = More pay
(Pays for quantity)
Program Strategy
Our program strategy consists of four components:
Healthier Populations
Improve the health status of North Dakotans by promoting healthy lifestyles, preventive care, disease management, & disparity elimination.
Better Outcomes
Improve access to quality healthcare at an affordable price to improve outcomes.
Better Experience
Enhance member & provider experience.
Smarter Spending
Increase effectiveness & efficiency in the delivery of healthcare programs & ensure value in healthcare contracts.
Program Start Date
July 1, 2023
Program Overview
Eligible Health Systems
Health systems with Prospective Payment System (PPS) hospitals are mandatory participants in the model.
As of July 1, 2023, the six health systems are: Altru Health System, CHI St. Alexius, Essentia Health, Sanford Bismarck, Sanford Fargo, and Trinity Health.
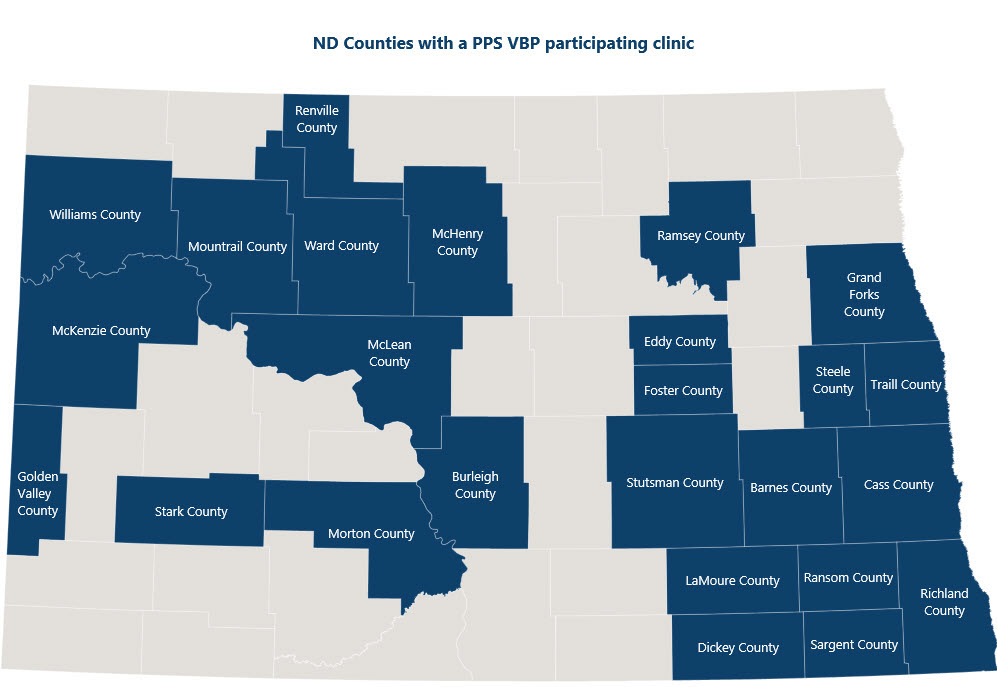
The map below of North Dakota shows the counties with a participating PPS VBP clinic in blue.
Structure
The PPS Health System VBP Program puts part of a hospital’s payment at-risk based on how well they perform on certain quality measures for their North Dakota Medicaid patients.
PPS Health Systems will not lose any funding if they meet the required performance goals.
Quality Measures
In the VBP Program, there are five main health care areas that focus on improving the overall health of the population. All of the measures chosen are connected to these areas.
- Primary Care Access and Preventive Care
- Maternal Health Services
- Behavioral Health Services
- Care of Acute and Chronic Conditions
- Oral Health Services
The Quality Measures for each program year are outlined below:
Program Requirements |
| Care Delivery Inventory Tool Submission |
| VBP Outcomes & Insights Meeting Participation |
| Supplemental Data Submission |
+
Pay for Performance |
| Breast Cancer Screening |
| Colorectal Cancer Screening |
| Child & Adolescent Well-Care Visit |
| Well-Child Visits First 30 Months of Life |
| Timeliness of Prenatal Care: Prenatal & Postpartum Care |
| Postpartum Care: Prenatal & Postpartum Care |
| Controlling High Blood Pressure |
| Plan All-Cause Readmissions |
| Topical Fluoride for Children |
+
Provisional Measures* No at-risk funds allotted |
| Postpartum Depression Screening |
| Depression Screening and Follow-up (Adolescents and Adults) |
| Glycemic Status Assessment for Patients with Diabetes |
Pay for Reporting |
| Submit Quality Improvement Plans through VBP Reporting Tool |
| VBP Quality Improvement Outcomes Meeting |
| Supplemental Data Submission |
+
Pay for Performance |
| Breast Cancer Screening |
| Child & Adolescent Well-Care Visit |
| Well-Child Visits First 30 Months of Life |
| Postpartum Care: Prenatal & Postpartum Care |
| Controlling High Blood Pressure |
| Plan All-Cause Readmissions |
| Topical Fluoride for Children |
| Screening for Depression & Documented Follow-up Plan |
| Ambulatory Care Emergency Department (ED) Visits |
FAQ
In 2026, Health Systems must complete the Program Requirements to be eligible for Pay for Performance.
Each quality measure gets an equal share of the total funds at-risk for the Health System. If a measure has more than one part, those funds are split evenly between each part. The amount of funding a provider earns for each measure depends on how well they perform compared to the Program Performance Target(s) shown below.
Full Creditno loss of funding if meeting the:
| Partial Creditonly partial loss of funding if:
| No CreditIf not meeting a Performance Target, participants will see a loss in funding. |
Any at‑risk dollars that are not earned go into the Redistribution Pool, which gives providers another chance to earn funding.
Starting in 2025, health system performance will be checked in two ways: how they compare to the Statewide Target and how they compare to their own past results. The Statewide Target is the level of performance the Department wants all providers in North Dakota to reach so that people receive high‑quality care. A Statewide Target is set for every measure.
Statewide targets are set based on what data is available and what level of improvement is reasonable. The targets follow this order:
- Use the National HEDIS 50th percentile, or another similar benchmark.
- Use the National Adult or Child Core Median.
- Use regional data if it is available.
- Use a target chosen by the state or an improvement over the system’s own past performance.
Performance periods follow the calendar year to match standard quality reporting. Because the program started in the middle of the year, the first performance period lasted 18 months. All current and future performance periods will last 12 months. The table below shows this and other important details for the first three performance periods.
| Program Period/At-Risk Timeframe | Quality Performance | Baseline Data Period | Performance Data Period | Payment Settlement Date |
|---|---|---|---|---|
| 7/1/2023 - 12/31/2024 | Pay for Reporting | Not applicable | 2023 & 2024 | 7/1/2025 |
| 1/1/2025 - 12/31/2025 | Pay for Reporting | Not applicable | 2025 | 7/30/2026 |
| Pay for Performance (Initial Measure Set) | 2024 | |||
| 1/1/2026 - 12/31/2026 | Pay for Performance | 2025 | 2026 | 7/30/2027 |
Contact Information
Medical Services Division
North Dakota Health and Human Services
600 E. Boulevard Ave., Dept. 325
Bismarck, ND 58505-0250
Email: dhsmedicaidquality@nd.gov
